Mental health practices across the USA are growing rapidly, but with that growth comes a hidden challenge—complex billing. From insurance claims to compliance with evolving regulations, billing services for mental health clinics have become a critical component of operational success. Many providers underestimate how much inefficient billing can impact revenue, patient satisfaction, and long-term sustainability.
This guide breaks down how modern mental health billing works, why outsourcing is gaining traction, and how clinics can streamline their processes without compromising care quality.
Why Mental Health Billing Is More Complex Than You Think
Unlike general healthcare billing, billing for mental health providers involves nuanced coding, session-based documentation, and strict payer-specific rules. Therapists, psychologists, and psychiatrists must deal with:
- Time-based CPT codes
- Frequent changes in insurance policies
- Authorization requirements for sessions
- Telehealth billing guidelines
- Medicare and Medicaid compliance
For example, billing Medicare for mental health services requires precise documentation and adherence to strict timelines. Even a small coding error can result in denied claims or delayed reimbursements.
This complexity is why many clinics are turning to specialized mental health billing services instead of handling everything in-house.
Understanding the Core of Mental Health Billing
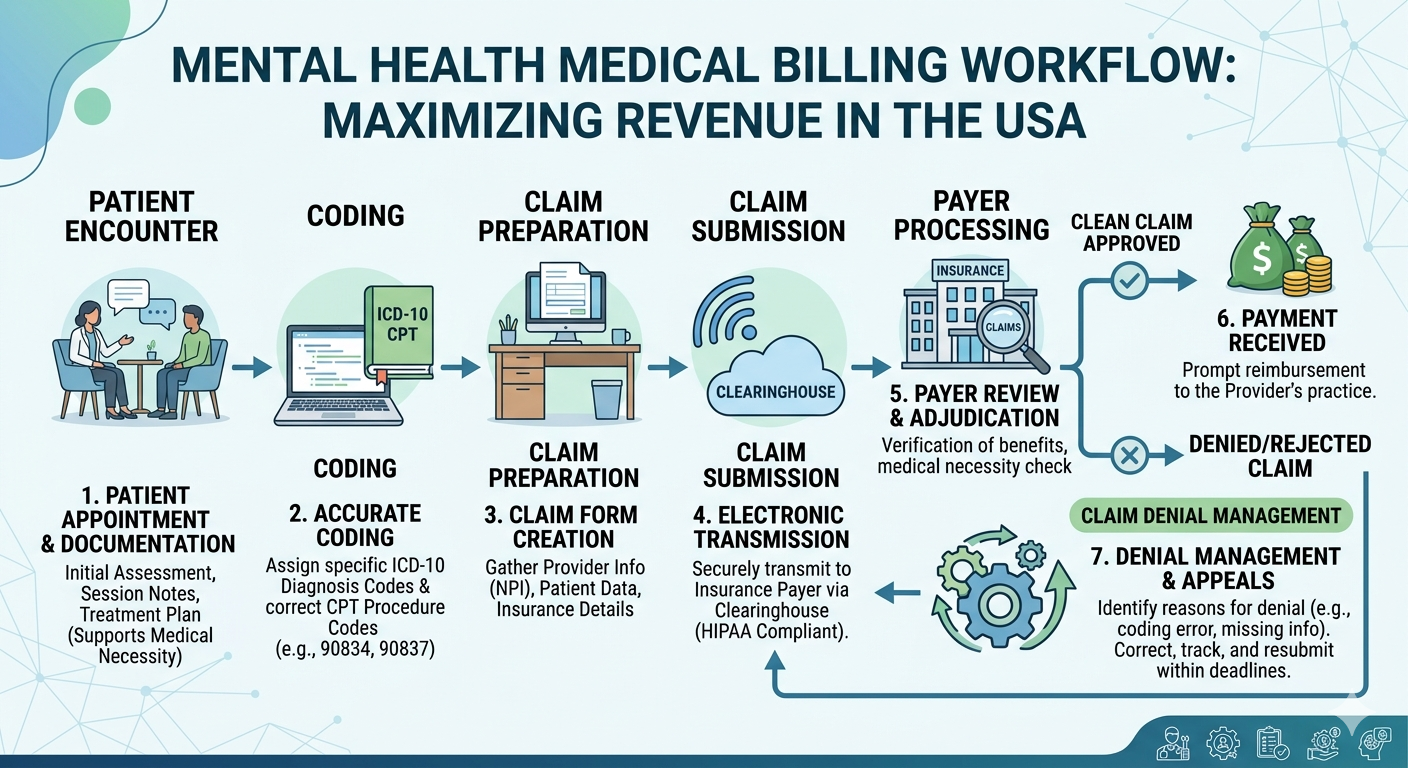
At its foundation, mental health medical billing includes several key steps:
1. Patient Registration and Insurance Verification
Before a session begins, accurate patient data and insurance verification are essential. Errors at this stage can cascade into claim denials later.
2. Coding and Documentation
Coding and billing for mental health services rely heavily on CPT and ICD-10 codes. Therapists must document session length, type, and diagnosis accurately.
3. Claim Submission
Claims must be submitted promptly and correctly formatted based on payer requirements.
4. Payment Posting and Denial Management
Tracking payments and addressing denied claims quickly ensures consistent cash flow.
5. Reporting and Optimization
Detailed reporting helps clinics identify revenue leaks and improve billing efficiency.
This entire process falls under revenue cycle management services, which aim to optimize every stage from patient intake to final payment.
Common Challenges in Billing for Mental Health Clinics
Even experienced clinics face recurring issues with billing for mental health services. Some of the most common challenges include:
- ❖ Frequent claim denials due to incorrect coding
- ❖ Delays in insurance reimbursements
- ❖ Lack of trained staff for mental health billing
- ❖ Compliance risks with HIPAA and payer guidelines
- ❖ Difficulty managing high patient volumes
For smaller practices, hiring and training an in-house billing team can be expensive and time-consuming. That’s where outsourcing mental health billing becomes a practical solution.
The Rise of Outsourced Billing for Mental Health
Outsourcing is no longer just a cost-saving tactic—it’s a strategic move. Clinics are increasingly partnering with experts who specialize in behavioral and mental health billing services.
Benefits of Outsourcing Mental Health Billing
- ✔ Improved Accuracy: Professionals stay updated with coding changes
- ✔ Faster Reimbursements: Clean claims reduce processing delays
- ✔ Reduced Administrative Burden: Staff can focus on patient care
- ✔ Scalability: Easily handle growth without hiring additional staff
- ✔ Compliance Assurance: Experts ensure adherence to regulations
For example, a mid-sized therapy clinic in Texas reduced its denial rate by over 30% within three months after switching to outsourced billing for mental health.
Key Features of Effective Mental Health Billing Solutions
Not all billing partners are created equal. The best mental health billing solutions offer a combination of technology and expertise.
What to Look For:
✔ Specialized Knowledge
Choose providers experienced in billing for mental health therapists and psychiatric services.
✔ Integrated Technology
Modern systems should support electronic health records (EHR) and automated claim tracking.
✔ Transparency
Detailed reports on claims, payments, and denials are essential.
✔ Credentialing Support
Mental health billing and credentialing services ensure providers are enrolled with insurance networks properly.
✔ Denial Management
A proactive approach to identifying and fixing issues before they impact revenue.
The Role of Medical Billing and Coding Services in Mental Health
Effective billing depends heavily on accurate coding. This is where medical coding services play a crucial role. Proper coding ensures:
- Correct reimbursement amounts
- Reduced claim rejections
- Compliance with payer policies
When combined with medical billing services, clinics benefit from a streamlined workflow that minimizes errors and maximizes revenue.
Additionally, comprehensive medical billing and coding services integrate seamlessly with revenue cycle management services, creating a complete financial ecosystem for the clinic.
Why Credentialing Matters More Than You Think
Many clinics overlook credentialing until it becomes a problem. Without proper credentialing services, providers cannot bill insurance companies, leading to lost revenue.
Credentialing includes:
- Enrolling providers with insurance networks
- Maintaining updated credentials
- Ensuring compliance with payer requirements
Delays in credentialing can cost clinics thousands of dollars in missed reimbursements. Integrating credentialing services with billing ensures a smoother process.
Medicare and Insurance Billing: What Clinics Need to Know
Billing Medicare for mental health services comes with strict rules. Clinics must ensure:
- Proper use of CPT codes for therapy sessions
- Documentation meets Medicare standards
- Timely submission of claims
- Compliance with telehealth policies
Private insurers also have varying requirements, making billing for mental health services even more complex. A single mistake can lead to audits or penalties.
Cost vs Value: Is Outsourcing Worth It?
Many clinic owners hesitate when considering a cheap outsource mental health billing company. While cost is important, value matters more.
In-House vs Outsourced Billing
| Factor | In-House | Outsourced |
|---|---|---|
| Cost | High (salaries, training) | Predictable monthly fee |
| Accuracy | Depends on staff | High (specialists) |
| Scalability | Limited | Flexible |
| Compliance | Risky | Managed by experts |
The best outsource mental health billing and coding services focus on long-term revenue growth rather than just cutting costs.
Real-World Example: How Efficient Billing Transforms Clinics
Consider a behavioral health clinic struggling with delayed payments and administrative overload. After implementing professional mental health billing services, they achieved:
- 40% reduction in claim denials
- Faster reimbursement cycles
- Improved patient satisfaction
- Increased focus on therapy quality
This transformation highlights how billing services for mental health clinics directly impact both financial health and patient care.
Choosing the Right Billing Partner
Selecting the right provider is crucial. Look for a partner that:
- Understands behavioral and mental health billing services
- Offers end-to-end solutions
- Provides transparent communication
- Has proven experience in medical billing for mental health
A reliable partner becomes an extension of your team rather than just a service provider.
Conclusion: Building a Sustainable Future for Mental Health Clinics
Efficient billing is no longer optional—it’s essential for survival in today’s healthcare landscape. Clinics that invest in professional billing services for mental health clinics gain a competitive advantage through improved revenue, reduced stress, and better patient outcomes.
Companies like 247 medical billing services are increasingly supporting mental health practices by offering integrated solutions that include medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services. These services work together to create a seamless billing ecosystem that allows providers to focus on what truly matters—patient care.
As mental health demand continues to rise in the USA, clinics that adopt smarter billing strategies will be better positioned to grow, adapt, and thrive.
FAQs
1. What are billing services for mental health clinics?
They are specialized services that handle insurance claims, coding, payment processing, and compliance for mental health providers.
2. Why is mental health billing different from general medical billing?
Mental health billing involves time-based coding, therapy session documentation, and unique payer requirements, making it more complex.
3. Is outsourcing mental health billing a good idea?
Yes, outsourcing improves accuracy, reduces administrative workload, and speeds up reimbursements.
4. What is included in mental health billing solutions?
It typically includes insurance verification, coding, claim submission, denial management, and reporting.
5. How do credentialing services help mental health clinics?
They ensure providers are enrolled with insurance companies, allowing clinics to receive reimbursements legally.
6. Can small clinics afford professional billing services?
Yes, many outsourced billing providers offer scalable and cost-effective solutions tailored to smaller practices.