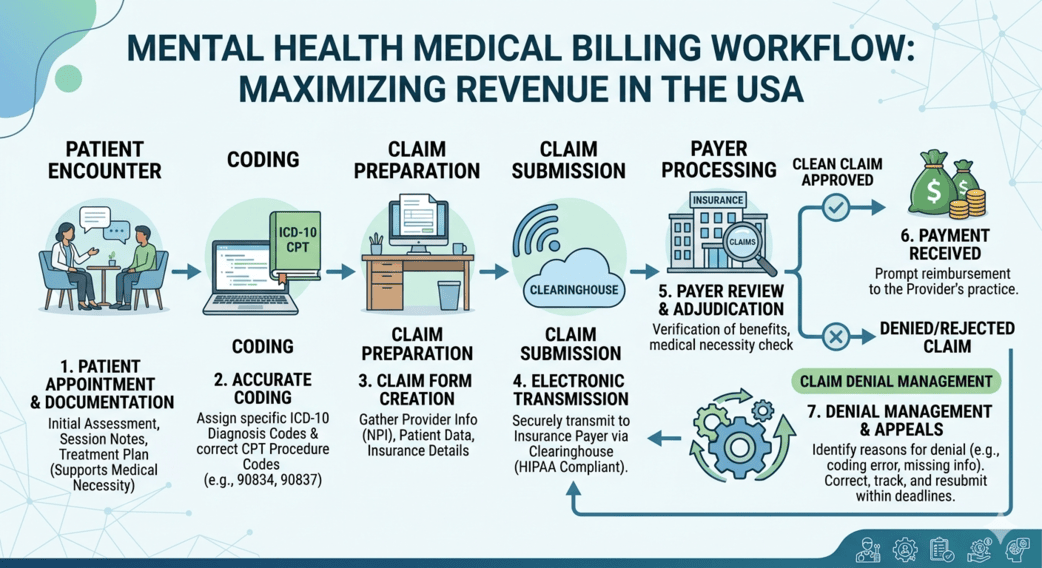
Mental health practices across the USA are growing rapidly, but so are the administrative challenges that come with them. Among the most complex tasks is billing for mental health providers—a process that directly impacts cash flow, compliance, and overall practice sustainability. From navigating insurance policies to ensuring accurate coding, even small errors can lead to delayed reimbursements or outright claim denials.
This guide breaks down everything mental health professionals need to know about billing, while also exploring how modern solutions and outsourcing strategies can simplify the process.
Understanding Billing for Mental Health Providers
Billing in mental health is not just about submitting claims—it’s a structured system involving documentation, coding, insurance verification, and follow-ups. Unlike other specialties, mental health billing often includes:
- Time-based CPT codes
- Frequent therapy sessions
- Pre-authorization requirements
- Changing payer rules
This complexity is why many providers rely on specialized mental health insurance billing services to manage their operations effectively.
Why Mental Health Billing is More Complex Than Other Specialties
Mental health billing differs significantly from general medical billing. Here’s why:
1. Time-Based Coding
Therapy sessions are billed based on duration, which requires precise documentation and coding accuracy.
2. Frequent Sessions
Unlike one-time procedures, patients often attend weekly or biweekly sessions, increasing billing volume.
3. Insurance Limitations
Many insurance providers impose session limits or require prior authorization.
4. Strict Documentation
Detailed notes must justify medical necessity, making compliance critical.
Because of these factors, working with a mental health billing specialist can significantly reduce administrative burden.
Key Components of Mental Health Medical Billing Services
A comprehensive mental health medical billing solution includes several interconnected processes:
Patient Eligibility Verification
Ensuring insurance coverage before appointments helps prevent denied claims.
Accurate Coding
Using correct CPT and ICD-10 codes is essential. This is where medical coding services play a vital role.
Claim Submission
Clean claims improve acceptance rates and speed up reimbursements.
Payment Posting
Tracking payments ensures transparency in financial records.
Denial Management
Identifying and correcting errors quickly helps recover lost revenue.
Follow-Ups
Consistent follow-ups with payers ensure timely payments.
These elements form the backbone of effective mental health medical billing services.
Benefits of Outsourcing Mental Health Billing Services
Many providers are shifting toward outsourced mental health billing due to increasing administrative pressure. Here’s why:
Reduced Administrative Workload
Outsourcing allows therapists to focus more on patient care rather than paperwork.
Improved Accuracy
A professional mental health billing and coding company ensures fewer errors in claims.
Faster Reimbursements
Experienced billing teams streamline claim processing.
Cost Efficiency
Hiring an in-house team can be expensive compared to outsourcing.
Compliance Assurance
Billing agencies stay updated with changing regulations and payer policies.
This is why many practices partner with a top outsource mental health billing company to optimize operations.
Choosing the Best Mental Health Billing Agency
Not all billing partners are created equal. When selecting the best mental health billing agency, consider the following:
Experience in Mental Health
General billing companies may not understand the nuances of therapy billing.
Technology and Tools
Advanced billing software improves accuracy and reporting.
Transparency
Clear reporting and communication are essential.
Custom Solutions
Look for agencies offering tailored mental health medical billing services outsourcing options.
End-to-End Services
From credentialing to collections, a full-service provider is ideal.
The Role of Credentialing in Mental Health Billing
Credentialing is often overlooked but plays a critical role in revenue generation. Without proper credentialing services, providers cannot bill insurance companies.
Credentialing involves:
- Enrolling with insurance networks
- Verifying provider qualifications
- Maintaining compliance with payer requirements
Delays in credentialing can lead to significant revenue loss, especially for new practices.
How Revenue Cycle Management Impacts Mental Health Practices
Revenue cycle management services (RCM) cover the entire financial process of a practice—from patient registration to final payment.
Effective RCM ensures:
- Fewer claim denials
- Faster reimbursements
- Better financial forecasting
- Improved patient billing experience
Combining RCM with medical billing and coding services creates a seamless workflow that enhances profitability.
Common Challenges in Billing Services for Mental Health Therapists
Even experienced providers face challenges such as:
Claim Denials
Incorrect coding or missing documentation often leads to rejections.
Insurance Verification Issues
Failing to verify benefits can result in unpaid claims.
Compliance Risks
HIPAA violations or incorrect billing practices can lead to penalties.
Time Constraints
Managing billing alongside patient care can be overwhelming.
These challenges highlight the importance of partnering with a reliable mental health billing services agency.
Real-World Example: How Outsourcing Improved Practice Revenue
A mid-sized therapy clinic in Texas struggled with delayed payments and frequent claim denials. After switching to outsourced mental health billing services, they experienced:
- 35% reduction in claim denials
- 25% faster reimbursement cycles
- Increased patient satisfaction due to transparent billing
This example shows how a structured mental health medical billing solution can transform practice operations.
In-House vs Outsourced Mental Health Billing
| Factor | In-House Billing | Outsourced Billing |
|---|---|---|
| Cost | High (salaries, training) | Lower, scalable |
| Accuracy | Depends on staff expertise | High with specialists |
| Compliance | Risk of errors | Managed by experts |
| Time | Time-consuming | Saves time |
| Technology | Requires investment | Included in services |
For many providers, outsourced mental health billing offers a more efficient and cost-effective approach.
Technology Trends in Mental Health Billing
The billing landscape is evolving with technology. Key trends include:
- AI-driven claim scrubbing
- Automated eligibility verification
- Cloud-based billing platforms
- Integrated EHR systems
These advancements are making billing services for mental health providers more efficient and reliable.
Integrating Medical Billing and Coding Services for Better Outcomes
Combining medical billing services with medical coding services ensures:
- Accurate claim submissions
- Reduced denials
- Better compliance
- Faster reimbursements
When these are integrated with revenue cycle management services, practices gain full control over their financial health.
Before You Choose a Mental Health Billing Partner
Ask these questions:
- Do they specialize in mental health billing companies?
- What is their claim acceptance rate?
- Do they offer end-to-end services including credentialing services?
- How do they handle denied claims?
- Can they scale with your practice growth?
The answers will help you identify the right mental health billing agency for your needs.
Conclusion
Billing for mental health providers in the USA is more than just an administrative task—it’s a critical component of practice success. With increasing complexity in insurance requirements and coding standards, relying solely on in-house processes can limit growth.
This is where experienced partners like 247 medical billing services can make a meaningful difference. By offering integrated medical billing services, medical coding services, medical billing and coding services, revenue cycle management services, and credentialing services, they help mental health practices streamline operations, reduce denials, and improve revenue flow—without adding extra stress to providers.
FAQs
1. What is billing for mental health providers?
It refers to the process of submitting and managing insurance claims for therapy and psychiatric services, including coding, documentation, and reimbursement tracking.
2. Why should I outsource mental health billing services?
Outsourcing reduces administrative workload, improves accuracy, ensures compliance, and accelerates reimbursements.
3. What does a mental health billing specialist do?
They handle coding, claim submission, denial management, and insurance follow-ups specifically for mental health services.
4. How do mental health billing companies improve revenue?
They minimize errors, reduce claim denials, and optimize the revenue cycle, leading to faster and higher reimbursements.
5. What is included in mental health medical billing services?
Services typically include eligibility verification, coding, claim submission, payment posting, denial management, and reporting.
6. Are credentialing services necessary for mental health providers?
Yes, credentialing is essential to enroll with insurance networks and legally bill for services, making it a crucial step in the billing process.