Mental health practices across Ohio are growing rapidly, but managing billing efficiently remains one of the biggest challenges providers face. From evolving insurance regulations to complex coding requirements, mental health billing Ohio demands precision, compliance, and strategic planning. Whether you are a solo therapist, group practice, or behavioral health clinic, understanding how billing works can directly impact your revenue and patient satisfaction.
This comprehensive guide explores everything you need to know about mental health billing in Ohio, including challenges, solutions, and how outsourcing can transform your practice operations.
Introduction
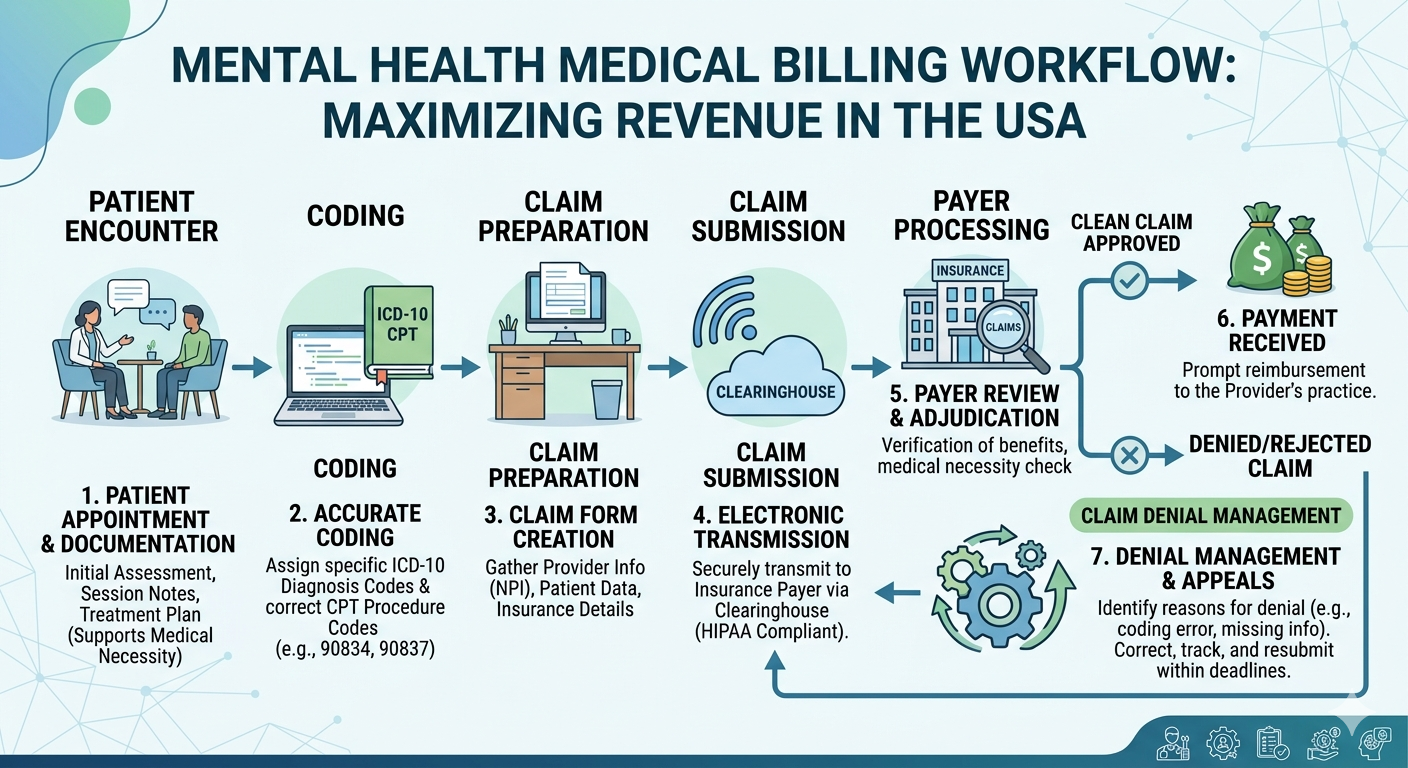
Mental health billing is not just about submitting claims. It involves a complete revenue cycle process that includes patient eligibility, coding accuracy, claim submission, denial management, and payment posting. In Ohio, where regulations and payer requirements vary, practices must adopt a structured approach.
Key Highlights:
-
Increasing demand for mental health services in Ohio
-
Complex payer policies and compliance requirements
-
Need for accurate coding and documentation
-
Growing trend of outsourcing billing services
-
Importance of revenue cycle optimization
Understanding Mental Health Billing in Ohio
Mental health billing Ohio involves specialized processes that differ from general medical billing. Behavioral health services often include therapy sessions, psychiatric evaluations, and medication management, each requiring specific CPT and ICD codes.
Providers in cities like mental health billing columbus ohio and mental health billing cleveland ohio often deal with multiple insurance providers, including Medicaid, Medicare, and private payers. Each payer has unique rules, making billing more complex.
Additionally, documentation plays a crucial role. Therapists must ensure that session notes align with billed services to avoid audits or claim denials.
Key Challenges in Mental Health Billing Ohio
Mental health providers face several operational and financial challenges when handling billing in-house.
1. Complex Coding Requirements
Behavioral health coding requires deep understanding of therapy types, session durations, and modifiers.
2. Frequent Claim Denials
Errors in eligibility verification or documentation often lead to rejected claims.
3. Changing Regulations
State-specific policies in Ohio can change frequently, impacting reimbursement rates.
4. Administrative Burden
Managing billing internally can take time away from patient care.
5. Insurance Variability
Different payers have different requirements, especially in urban areas like mental health billing columbus.
Importance of Accurate Coding and Documentation
Coding accuracy is the backbone of successful mental health billing. Even minor errors can lead to claim rejections or compliance issues.
For example:
-
Incorrect session duration codes
-
Missing modifiers for telehealth services
-
Incomplete patient documentation
Practices in regions similar to mental health billing massachusetts or mental health billing in chicago often adopt strict documentation protocols to maintain compliance. Ohio providers can benefit from implementing similar standards.
Benefits of Outsourcing Mental Health Billing
Outsourcing has become a preferred solution for many mental health providers. Instead of managing billing internally, practices partner with experts who specialize in behavioral health billing.
Advantages include:
-
Reduced administrative workload
-
Improved claim acceptance rates
-
Faster reimbursements
-
Compliance with state and federal regulations
-
Access to experienced billing professionals
Many providers compare services across states, such as outsourcing mental health medical billing services provider in florida or mental health billing in san diego, to find best practices and scalable solutions.
Choosing the Right Mental Health Billing Service
Selecting a reliable billing partner is critical for long-term success. Not all billing companies offer the same level of expertise or service quality.
When evaluating options, consider:
-
Experience in behavioral health billing
-
Knowledge of Ohio-specific regulations
-
Transparent pricing models
-
Strong denial management process
-
Use of advanced billing software
Practices often research providers beyond their state, including best mental health billing services company new jersey or professional mental health billing company rhode island, to benchmark service quality and performance.
Mental Health Billing Trends in Ohio
The mental health billing landscape is evolving rapidly. Providers must stay updated with the latest trends to remain competitive.
Telehealth Expansion
Teletherapy services have increased significantly, requiring updated billing practices.
Value-Based Care Models
Reimbursement is shifting from volume to quality-based care.
Automation and AI Tools
Billing systems are becoming more efficient with automation.
Cross-State Benchmarking
Providers compare services like mental health billing services new jersey and mental health billing services pennsylvania to improve efficiency.
How Billing Impacts Revenue Cycle Management
An optimized billing process directly affects your revenue cycle. Delays or errors in billing can disrupt cash flow and impact overall profitability.
Efficient billing ensures:
-
Faster claim submissions
-
Reduced denial rates
-
Accurate payment posting
-
Improved financial reporting
Providers offering billing services for mental health providers texas or billing services for mental health providers new york often integrate advanced revenue cycle strategies that Ohio practices can adopt.
Comparing Billing Services Across States
While focusing on mental health billing Ohio, it is helpful to compare services offered in other states to identify best practices.
For instance:
-
best mental health billing company north carolina emphasizes compliance and automation
-
best mental health billing company south carolina focuses on cost efficiency
-
cheap mental health billing company south carolina and cheap mental health billing company virginia provide budget-friendly options
-
billing services for mental health providers pennsylvania and billing services for mental health providers washington highlight scalable solutions
These comparisons help Ohio providers choose the most suitable billing approach.
Steps to Improve Mental Health Billing Efficiency
Improving billing efficiency requires a structured approach.
1. Verify Patient Eligibility
Always confirm insurance coverage before appointments.
2. Use Accurate Coding
Ensure correct CPT and ICD codes are applied.
3. Maintain Detailed Documentation
Keep thorough records of patient interactions.
4. Submit Claims Promptly
Avoid delays in claim submission.
5. Monitor Denials
Analyze and resolve rejected claims quickly.
6. Consider Outsourcing
Partnering with experts can significantly improve outcomes.
Why Ohio Providers Are Moving Toward Outsourcing
Mental health practices in Ohio are increasingly outsourcing their billing processes. The reasons are clear:
-
Rising operational costs
-
Need for specialized expertise
-
Increased patient volume
-
Demand for faster reimbursements
Outsourcing allows providers to focus on patient care while experts handle the financial side of the practice.
Conclusion
Mental health billing Ohio is a complex but essential component of running a successful behavioral health practice. From coding accuracy to compliance and revenue optimization, every step in the billing process matters.
By adopting best practices, leveraging technology, and considering outsourcing, providers can significantly improve their financial performance. Partnering with an experienced team like 247 Medical Billing Services can make a meaningful difference. Their expertise in medical billing services, medical coding services, medical billing and coding services, revenue cycle management, and credentialing services ensures a streamlined and efficient billing process tailored to mental health providers.
FAQs
What is mental health billing Ohio?
Mental health billing Ohio refers to the process of coding, submitting, and managing claims for behavioral health services provided within the state.
Why is mental health billing different from general medical billing?
It involves specialized codes, therapy session documentation, and unique payer requirements specific to behavioral health services.
How can I reduce claim denials in mental health billing?
Ensure accurate coding, verify insurance eligibility, and maintain proper documentation for every patient encounter.
Is outsourcing mental health billing beneficial?
Yes, outsourcing improves efficiency, reduces errors, and allows providers to focus more on patient care.
What should I look for in a billing company?
Choose a company with experience in behavioral health, knowledge of Ohio regulations, and a strong track record in denial management.
Can small practices benefit from professional billing services?
Absolutely. Even small practices can improve revenue and reduce administrative workload by using professional billing services.
How does billing impact revenue cycle management?
Accurate and timely billing ensures steady cash flow, reduces denials, and improves overall financial health of the practice.